Excellent study material for all civil services aspirants - begin learning - Kar ke dikhayenge!
mRNA: HOPE AND HYPE
Read more on - Polity | Economy | Schemes | S&T | Environment
- It is a decades-old idea, but what suddenly made the mRNA vaccine practicable in 2020-21 was the convergence of many technologies.
- In April 2021, the government of India said it had approved Pune-based Gennova Biopharma, a subsidiary of Emcure Pharmaceuticals, that produces recombinant drugs, to go ahead with Phase I and II human clinical trials of its vaccine called HGCO19.
- If Gennova gets it right, it would win global recognition and stand shoulder-to-shoulder with Pfizer and Moderna.
- Gennova’s vaccine is of a type that is being hailed as a rising star in the world of vaccinology — ‘mRNA’ (messenger RNA), which is a fruit of three decades of research.
- Why is mRNA different — and better?
- Conventional vaccines are essentially weakened pathogens (or disease-causing microbes) introduced into the body to provoke the immune system to launch a response — namely, produce the appropriate antibodies (aka immunoglobulins, which are Y-shaped proteins that engulf the invaders and destroy them). While doing so, the immune system learns all about the pathogen; now it is ready for a real attack.
- Since you are introducing a disease causer, side effects are inevitable. mRNA works differently.
- Take a pathogen like a virus, which has a ‘core’ of genes made of DNA or RNA (SARS-CoV-2 has RNA). These genes are wrapped in a coat of proteins.
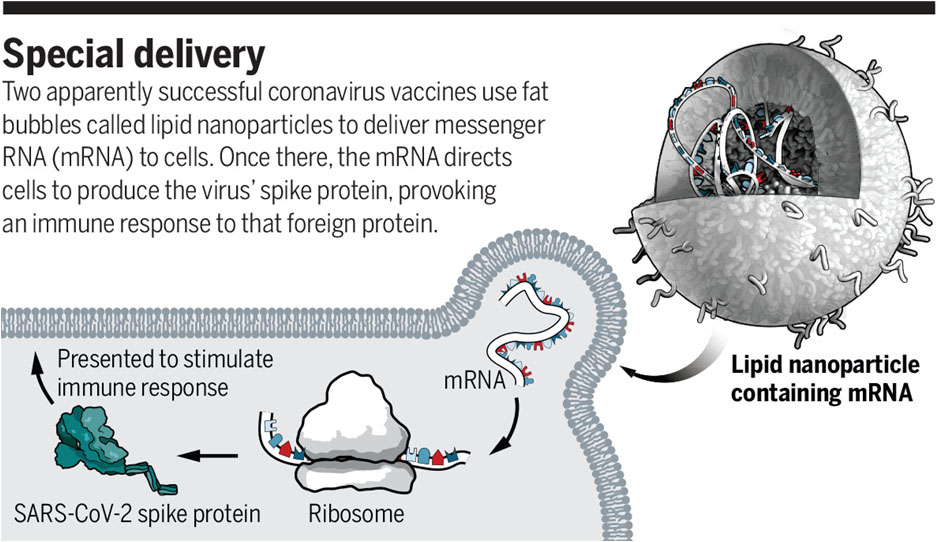
- To make the coat, the DNA or RNA genes of the virus make a ‘messenger RNA’, which contains the instructions for it.
- An mRNA of a particular pathogen makes a protein of a particular structure. In the case of SARS-CoV-2, the coat has ‘spike’ proteins.
- The mRNA vaccine developers make this particular mRNA in the lab. You inject this synthetic mRNA, you trick the immune system into believing that it is actually a pathogen. An immune response is triggered, antibodies are produced. Job done.
- What works – There are many advantages with the mRNA vaccine.
- It introduces no attenuated pathogen into the body, so no side-effect.
- It is synthesised in the lab, requiring no host such as eggs or bacteria, so scaling up is easy.
- The mRNA vaccines are also believed to help produce ‘adjuvants’ — substances that enhance the immune system’s response.
- There are the diseases where conventional vaccines have failed — HIV-1, herpes simplex virus and respiratory syncytial virus (RSV). Furthermore, development of a vaccine up to the marketing stage takes time; diseases overwhelm us before we find one, as seen in the case of Ebola and Zika viruses.
- A 2018 paper in Nature said that “preclinical studies have created hope that mRNA vaccines will fulfil many aspects of an ideal clinical vaccine”.
- mRNA vaccines can be produced relatively easily and quickly. Pfizer and Moderna have since come up with mRNA vaccines and others, such as Gennova, are working on it for Covid-19.
- Some others are bringing mRNA vaccines for other diseases (Argo Therapeutics, Erasmus, Massachusetts General Hospital and McGill University for HIV-1; Moderna for Zika and Influenza).
- Many Indian vaccine manufacturers have mRNA in their to-do list. But experts have also cautioned against explosive optimism. There are still some challenges.
- Challenges – The ‘immunogenicity’ — the ability to provoke an immune response — is yet to be fully understood.
- Will it trigger unwanted immune response? The stability of mRNA inside the cells has also been a challenge, as it quickly disappears.
- Another unknown is whether the mRNA vaccine will create immunity that lasts as long as conventional vaccines? What kind of refrigeration and handling will mRNA vaccines require?
- Current research is on tackling these challenges. Some success has been achieved in areas such as delivery into cells and refrigeration.
- Cutting edge - There is really not much of a track record (of mRNA vaccines) beyond their remarkable success with Covid-19.
- Observers note Indian companies are not far behind in this cutting-edge technology.
- Gennova was already into mRNA when the pandemic broke out.
- When other companies too jump in, it would do a world of good, because mRNA is good for both infectious and non-infectious diseases, notably cancer.
- Cancer cells make proteins, which can also be targeted by mRNA vaccines.
- By all accounts, the time for the mRNA vaccine seems to have arrived.
- Experts stress that while mRNA’s use as a vaccine was deduced decades ago, the convergence of disparate technologies (engineering and manufacturing mRNA in a lab, delivery into cells, storage) is happening now, making the vaccine practicable.
- The future of mRNA vaccines is extremely bright, and the clinical data and resources provided by companies and other institutions are likely to substantially build on and invigorate basic research into mRNA-based therapeutics.
* Content sourced from free internet sources (publications, PIB site, international sites, etc.). Take your own subscriptions. Copyrights acknowledged.